BC medical covers a portion of your eye examination if you have underlying systemic disease, such as diabetes, or ocular disease including cataracts or glaucoma.
See Optical Insurance
Macular degeneration is a degenerative process which disturbs this delicate, highly specialized tissue. It is linked to smoking, genetics, diet, light exposure and poor health. Untreated macular degeneration is one of the leading causes of blindness in those over 65 years old.
Age related macular degeneration is a potentially visually devastating disease that affects your central vision. Your prognosis depends on the form and severity of the disease as well as your risk factors.
As you age it is important to check your eyes for the presence of macular changes. There are vitamins, diet and lifestyle changes that you can make to change the course of macular degeneration.
The macula of the eye refers to the small central area of the retina which is highly specialized to resolve detail. This tiny area is our 20/20 sweet spot which we need to see any small detail including reading a book or seeing detail on a person’s face.
Early macular degeneration is often asymptomatic and can only be detected through an eye examination. Early symptoms can include blurry, cloudy or distorted central vision. In advanced stages, central vision loss can be severe.
Once early macular degeneration is recognized, you should have your eyes examined every 6-12 months, depending on the severity. If you notice a sudden change to your central vision, it is very important that we see you right away.
While researchers have not yet discovered a cure for dry age-related macular degeneration, there are treatment options which prevent the disease from progressing to blindness. It’s important to have an open discussion with your eye doctor about the risks and limitations of the different treatments.
Wet macular degeneration is the more severe form of the disease. If this is detected during your examination you will be referred promptly to a retinal ophthalmologist. This is treated by the injection of a medication directly into the eye inhibit blood vessel growth.
A cataract is clouding that develops in the lens at the front of the eye. It is usually related to aging, but can also affect you at a much younger age.
Cataract progression is influenced by aging, genetics, UV/blue light exposure, trauma and non-optimal blood sugar levels.Cataracts are caused by a clouding in the crystalline lens of the eye which is located just behind the iris. A cataract generally causes a gradual decline in your vision causing your vision to become blurry and dim. However, some cataracts progress very rapidly as well.
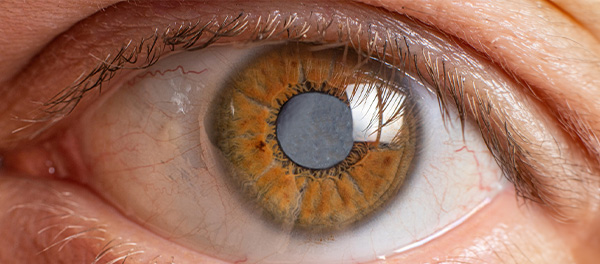
Cataracts are fairly easy to detect using a slit lamp evaluation during your comprehensive eye exam. When your cataracts are compromising your vision enough to significantly affect your day to day visual needs or are causing annoying glare and difficulty seeing at night, they are ready to come out. When your cataracts are ready to be removed, we will refer you to a local ophthalmologist for a surgical consult.
Ophthalmologists perform cataract extraction when they are ready to be removed. Cataracts are treated by small incision surgery in which your lens is replaced by an artificial lens. Although cataract surgery is usually successful, it is important to remember than it is not without risk.
We will perform an eye examination about 6 weeks after your cataract surgery to determine your new prescription and ensure that there are no complications from the surgery.
Glaucoma is a disease that causes irreversible damage the optic nerve of the eye, resulting in vision loss. It is often asymptomatic in the early stages, and only a comprehensive eye exam can determine if you have or are at risk for developing glaucoma.
Early detection of glaucoma is key to having a successful outcome. Your optometrist will determine if you are at risk for glaucoma during your examination and may need to order additional specialized testing. Glaucoma is a complex disease, and baseline data is needed to monitor for progression over time.
At Summerland Optometry we have advanced technology to detect glaucoma at an early stage. To monitor our patients for glaucoma we measure their eye pressures, and their corneal thickness. We also obtain a detailed optic nerve scan (OCT), and test for peripheral vision loss (Visual field). OCT nerve scans and visual field testing are necessary for the diagnosis and management of glaucoma.

Diabetes is a very common condition in our society. Unfortunately, it can put you at increased risk for developing many eye conditions including diabetic retinopathy, diabetic macular edema, glaucoma, and cataracts.
If you are diabetic you know and understand how important it is to control your blood sugar levels to ensure they are stable. Because diabetes is a vascular disease, it is very important for diabetics to have annual exams.
In a comprehensive eye exam, we will look closely at your retinal blood vessels which reflect the state of your capillary circulation in your entire body. The retina is the only place in the body where capillaries can be easily viewed. With wide field retinal imaging (Optomap) and cross-sectional macular scans (OCT), we can pick up early vascular anomalies and alert your medical physicians of our findings. In fact, when we see a diabetic for routine examination, we always send a report to your family doctor of our ocular findings.
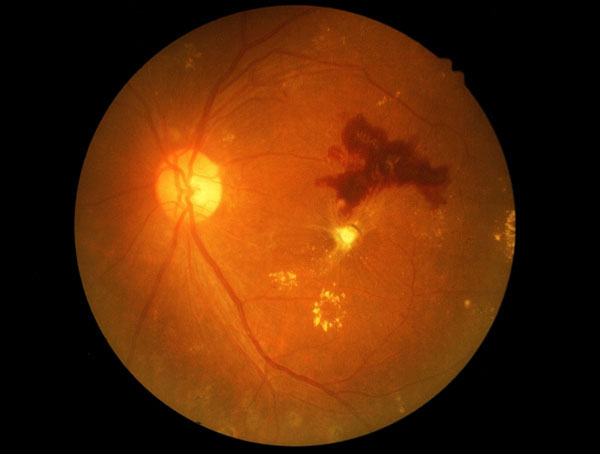
If your diabetes is not optimally controlled or you have had the disease for many years, we often see diabetic retinopathy in your eyes. Blood vessels can leak blood and fluid into the eye and even grow new abnormal vessels. Diabetic retinopathy can cause permanent vision loss and often treatments are required.
Macular edema occurs when fluid accumulates at the macula from leaky blood vessels. Your macula is the central part of your retina responsible for central vision; therefore, damage to this area can be devastating. Macular edema is visualized on our cross-sectional macular scan (OCT). Referrals are often required to retinal ophthalmologists for treatment.
The sudden onset of flashes and floaters is a common reason why patients report for urgent evaluations. These ‘flashes and floaters’ can be a very normal part of your eyes’ aging process, but any new symptoms can indicate a problem and need to be assessed in a timely manner.
Flashes are odd perceptions of light usually in the side vision that seem to come out of nowhere. Floaters are shadowy forms that seem to drift in the vision. They are best observed when looking at a light background that has no detail such as a light wall or in dense fog.
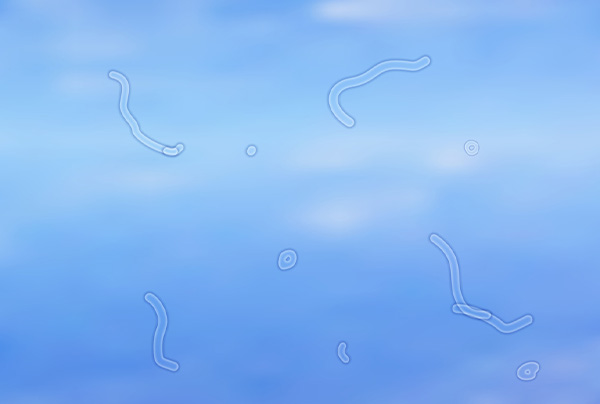
Flashes and floaters of acute onset are usually cause by an acute event called a vitreous detachment which is a normal age-related change.
A vitreous detachment occurs when the jelly in the back cavity of the eye, the vitreous gel, shrinks and separates from the retina. The vitreal gel can sometimes pull on the retina, and this traction lead to flashes of light. The floaters are seen when you can view the back of the vitreous gel.
If you experience any new symptoms of flashes or floaters you should have your eyes checked promptly. The tractional effect on the retina can cause a retinal tear and this needs to be treated ASAP. A retinal tear keeps progressing until treated with laser or surgery and can lead to a retinal detachment in worst case scenarios.
The information below applies to all the information contained on the summerlandoptometry.ca Website.
The users of this Website agree to comply with the terms set out below.
Summerland Optometry owns and operates a Website at summerlandoptometry.ca (hereinafter referred to as the “site” or “Website”). Unless specified otherwise on the site, it is accessible to all users (hereinafter, the "user"). Refrain from using this Website unless you agree to comply with the conditions.
Information on this Website is intended for informational purposes only and has no contractual value. Summerland Optometry reserves the right to modify the content of this site. At any time, without prior notice. Summerland Optometry assumes no liability for errors or omissions in the content of this Website or for information reliability or completeness of said information.
Information published on this Website is based on marketing, statistical or commercial services or other sources the Summerland Optometry considers reliable and are the sole responsibility of their authors and not of Summerland Optometry. We do not assume any liability for the accuracy or completeness of said information and in no circumstance should this information be regarded as such. Opinions and information as presented on this site reflect our position as of the date of publication and are subject to change without notice.
Summerland Optometry, its employees and directors will not be liable for damages incurred as a result of the information published on this site, for the views and advice published, expressed or implied regardless of its nature.
Summerland Optometry expressly refuses any and all responsibility for the manner in which the user of the site may use the information contained, in any decisions that may be made and in the actions that may or may not be taken based on said information.
Presentations made and contained on this site are the intellectual property of Summerland Optometry. Reproduction in whole or in part of this site on any other medium in prohibited without the express permission of Summerland Optometry.
User may solely use the information contained on this site for personal use. Reproduction in whole or in part of said information on paper may only be performed for personal use. Said information is not to be copied, distributed or transmitted to third parties nor may it be inserted in a document or other medium.
The links to external Websites and their content shall not be prejudged and Summerland Optometry will in no way be held responsible for any direct or indirect prejudice that may result from gaining access to and usage of said sites.
Summerland Optometry draws the attention of the user to the fact that all communication transmitted through this Website remains in the public domain and not the private domain. Summerland Optometry cannot accept responsibility for the security of the transmission of information.
The confidentiality and integrity of the information circulating over the internet cannot be ensured. Summerland Optometry cannot accept responsibility in the case that data contained on this site is intercepted.
Summerland Optometry site uses cookies. These cookies are small text files saved on the hard disk of a user's computer. These files are completely harmless and cannot contain viruses. These cookies are used to analyze visits to the site. Summerland Optometry calls upon Google Analytics to help track how users use the site. The number of visitors, path taken to access the site and length of each visit are measured. The cookies cannot, in any way, identify the user. All data is completely anonymous and compiled solely for the purpose of improving the site and tailoring the content to the needs of its visitors.
The person responsible for the protection of personal information is the owner of : Summerland Optometry
Summerland Optometry makes no representations that the content of this site is free of infections, viruses, worms, Trojan horses and/or other codes with contaminating or destructive properties. It is the user's responsibility to take protective measures.
Under no circumstances shall Summerland Optometry be held responsible for transmission errors of any sort, such as loss of or damage to data, or changes of any type whatsoever, including direct or indirect damage resulting from the use of the services provided on this site.
This Agreement shall be governed by and construed in accordance with the laws of the province of British Columbia.
Any dispute arising of this Agreement shall be brought before the court in the judicial district of
Summerland Optometry's head office.
Address:
13225 N Victoria Road
Summerland, BC
V0H 1Z0;
Tel: 250 494-9266.
Summerland Optometry
13225 N Victoria Road
Summerland, BC
V0H 1Z0
Tel: 250 494-9266
Thank you for visiting summerlandoptometry.ca (the “Website”), provided to you by Summerland Optometry (“We”). We respect the privacy of every individual who visits the Website and are sensitive to privacy issues on the Internet. We believe it is important that you know how we deal with information received about you.
This privacy policy (the “Privacy Policy”) explains how we collect, use, disclose, and protect the personal information of our customers and Website users ("you"), describes the types of information we may collect from you or that you may provide to us, and our practices for collecting, using, maintaining, protecting, and disclosing that information. The Website is for general audiences and is not specifically targeted to or intended for use by children.
We will only use your personal information in accordance with this Privacy Policy unless otherwise required by applicable law. We take steps to ensure that the personal information that we collect about you is adequate, relevant, not excessive, and used for limited purposes. Privacy laws in Canada generally define "Personal Information" as any information about an identifiable individual, which includes information that can be used on its own or with other information to identify, contact, or locate a single person.
By accessing or using the Website, you are accepting the practices described in this Privacy Policy, and you are consenting to our processing of your information as set out in this Privacy Policy. We may modify or update this Privacy Policy from time to time; if we change this Privacy Policy in a manner that materially impacts your privacy rights, we will provide a notice to you. Your continued use of the Website or our services after any modification to this Privacy Policy will constitute your acceptance of such modification. However, when required by law, we will confirm your consent to the revised Privacy Policy terms. This Privacy Policy is incorporated into and considered a part of the Website Terms and Conditions of Use, located here
We collect and use several types of information from and about you, including:
The information we collect directly from you may include:
We use your information, including your Personal Information, to manage our business and to maintain and develop commercial relationships with you. We will collect, use, and disclose such information only to the extent that is necessary for those purposes.
We use information that we collect about you or that you provide to us, including any Personal Information:
We may partner with Microsoft Clarity and Microsoft Advertising to capture how you use and interact with our website through behavioral metrics, heatmaps, and session replay to improve and market our products/services. Website usage data is captured using first and third-party cookies and other tracking technologies to determine the popularity of products/services and online activity. Additionally, we use this information for site optimization, fraud/security purposes, and advertising. For more information about how Microsoft collects and uses your data, visit the Microsoft Privacy Statement.
We will not rent or sell your information to third parties without your consent. We only share your data as specifically provided in this Privacy Policy.
In addition to any disclosure you may have consented to or permitted under the terms of this Privacy Policy, we may transfer your data, including Personal Information to third parties in the following limited circumstances:
We are committed to protecting the confidentiality, integrity, availability and privacy of your Personal Information. We have put appropriate physical, technological and procedural security measures in place designed to help prevent your Personal Information from being lost, used, modified or accessed in an unauthorized way, or improperly disclosed. Examples of such measures include restricted access to offices, training of personnel, using passwords and well-defined internal policies and practices. We also use encryption technology and Secure Socket Layers ("SSL") in all areas of the Website where your personal account information is required.
In addition, we limit access to your Personal Information to those employees, agents, contractors and other third parties who have a business need-to-know. They will be required to process your Personal Information only on our instructions and they are subject to an obligation of confidentiality. Our service providers are required to maintain adequate security protections in place designed to help safeguard your Personal Information and are not permitted to use it for any purpose other than fulfilling services to us.
If you have any questions about securing your personal data, please contact us in accordance with the “How to Contact Us” section below.
We will retain your Personal Information for as long as it is needed:
We may retain non-personal information that has been sufficiently aggregated or anonymized for a longer period.
Once the retention period is over, we will dispose of your Personal Information as provided for in our internal data retention and disposal policy.
We use facilities operated by "Amazon Web Services" and located in Canada as our information storage and processing infrastructure. Our service providers can also, from time to time, store your Personal Information in accordance with purposes outlined in this Privacy Policy.
If you have any questions about this Privacy Policy, you can contact us at 250 494-9266.